
March 2017
General News
John Naylor named new Medica CEO and president
Medica recently announced the retirement of CEO and President David Tilford. John Naylor, who had served as senior vice president of Medica's commercial markets division, was named as Tilford's successor, assuming the new role immediately. Tilford had led Medica for 16 years.
"I am delighted to take over the reins from David and am confident that he leaves the organization positioned well for success in the constantly changing health care industry," Naylor said.
Naylor joined Medica in April 2010 and has more than 30 years of industry experience. He had led the commercial markets division for more than four years and is responsible for several innovations. Chief among them is the development of accountable care organization products with several health care systems including Altru, Essentia Health, Fairview/North Memorial, HealthEast, Mayo Clinic Health System, Park Nicollet and Ridgeview Community Network.
Prior to joining Medica, Naylor was with Willis Towers Watson (formerly Towers Perrin) for 21 years. For more than a decade, he served as the market leader for the Towers Perrin Minneapolis office and managing director for the U.S. Central Region, with responsibility for all aspects of selling and providing service to clients across the company’s human resources consulting practice.
Medica Foundation announces provider grant recipients
2016 core mission support grants total $200,000
The Medica Foundation has concluded its organizational core mission support funding for 2016, awarding grants totaling $200,000 to 40 nonprofit agencies. Grants were awarded to support health-related programming that is essential to each organization’s nonprofit mission. This funding was provided to organizations in the regional and rural areas of Medica’s service area which includes Minnesota, Western Wisconsin, North Dakota and South Dakota. Selected organizations operate outside of the Twin Cities metro area and are dedicated to supporting the health of those they serve.
The following providers were among the recipients of core mission grants of up to $5,000 each:
- Catholic Social Services (Rapid City, S.D.) – to support the Counseling and Family Services departments
- Duluth Lighthouse for the Blind (Duluth, Minn.) – to boost one-on-one services to seniors, reducing health risks and promoting aging in place
- Le Sueur County (Le Center, Minn.) – to support the Healthy Smiles program
- Northern Dental Access Center (Bemidji, Minn.) – to leverage other grant contributions to purchase dental supplies for more than 250 patient appointments
- ShareHouse (Fargo, N.D.) – to provide 250 hours of recovery coaching time
- VINE Faith in Action (Mankato, Minn.) – to target outreach to elders including transportation, interpreter fees, sliding-fee discounted memberships, and culturally appropriate classes
- Women's Health Center of Duluth (Duluth, Minn.) – to purchase supplies for medical appointments
- Zumbro Valley Health Center (Rochester, Minn.) – to provide under- and un-served populations with high-quality mental, chemical and medical care
In total for 2016, the Medica Foundation awarded $1,222,000 to 96 nonprofit and government agencies. “Health care is going through a period of change and we remain committed during these challenging times through support of our partners who improve health and remove barriers to health care services for those in need,” said JoAnn Birkholz, director of the Medica Foundation.
Details about grant recipients, funding opportunities, giving guidelines and application deadlines are available online at medicafoundation.org.
Reminder:
Annual ‘Disclosure of Ownership’ forms needed
Any providers who have not yet completed and returned their “Disclosure of Ownership Statement” should do so as soon as possible. It is past due. It can be returned to Medica by e-mail. Providers also received this annual request by U.S. mail last month. Each year, providers must complete and submit an updated disclosure form in accordance with regulatory agency requirements.
As a reminder, providers who see patients covered under Medica products for government programs need to complete and return the Disclosure of Ownership Statement to Medica annually. This step is necessary for Medica to comply with contracts it holds with both the Centers for Medicare and Medicaid Services (CMS) and the Minnesota Department of Human Services (DHS).
Medica wishes to thank providers for their time, especially those who promptly responded to this obligation. More details about this compliance requirement are available in the Medica Provider Administrative Manual.
(Update to "Annual ‘Disclosure of Ownership’ forms needed soon" article in the January 2017 edition of Medica Connections.)
Effective March 12, 2017:
By mid-March, NDC, NDC units needed with HCPCS codes
As previously published, Medica will expand a requirement for claims that include drug codes to also include corresponding national drug code (NDC) numbers and NDC units of measure along with the Healthcare Common Procedure Coding System (HCPCS) code. This change will be effective with March 12, 2017, dates of service. As a reminder, this new requirement will be expanded to all Medica claims, including those for commercial, individual and family business (IFB) and Medicare products. As part of this new requirement, Medica will reject claims with HCPCS drug codes if they lack NDC numbers and NDC units of measure.
This change will apply to both physician and facility claims for all Medica products. If providers have a claim rejected due to this new claim requirement (or claim edit), they will need to correct their claim and resubmit it so that the claim can be processed.
(Update to "All claims with HCPCS drug codes to require NDC, NDC units" article in the January 2017 edition of Medica Connections.)
Effective by April 1, 2017:
New icons to display for Premium physician designations
Medica is now preparing for the 2017 Premium Designation program, which conveys quality and cost-efficiency designations for physicians as part of the provider search tool on medica.com. Soon, there will be interim changes for this program:
- New Premium program heart icons will replace the current text-only designations. Although physician designations are staying the same for now, the table below shows how the Premium program designations will display publicly on the Medica online physician directory.
- Ophthalmology will no longer be included as a specialty in the Premium program. There will be a total of 26 specialties going forward.
Here are the new icons and what they mean.
| Designation |
Description |
Premium Care Physician

|
The physician meets the criteria for providing quality and cost-efficient care. |
Quality Care Physician

|
The physician meets the criteria for providing quality care and does not have enough claims data to be evaluated for cost-efficient care.
The physician meets the criteria for providing quality care and does not meet the criteria for cost-efficient care.
|
|
Quality Not Evaluated
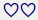
|
The physician’s specialty is not evaluated or the physician‘s evaluation is in process.
The physician does not have enough claims data to be evaluated for quality, so the physician is not eligible for the cost-efficient care designation.
|
|
Does Not Meet Quality

|
The physician does not meet the criteria for providing quality care so the physician is not eligible for the cost-efficient care designation.
|
These changes on medica.com are expected to take place by April 1, 2017. Then, later in 2017, there will be a transition to a new program year. Physicians included in the 2017 Premium program will receive a letter notifying them of their latest designation, program changes for this year, and how to log in to see their reports.
[Return to top]
Clinical News
Effective May 1, 2017:
Medica to implement new coverage policies
The following benefit determinations will be effective beginning with May 1, 2017, dates of service. These new policies will apply to all Medica products including government products unless a particular health plan (whether commercial, Medicare or Medicaid) requires different coverage.
Corneal cross-linking
Medica has reviewed corneal cross-linking (CXL) and has made the following determinations:
- Conventional and accelerated corneal cross-linking for the treatment of keratoconus and corneal ectasia will be covered.
- Conventional and accelerated corneal cross-linking for all other indications is investigative and therefore will not be covered.
- Transepithelial and partial epithelium-off corneal cross-linking is investigative and therefore will not be covered.
CXL is a procedure that combines the use of ultraviolet (UV) light and riboflavin (vitamin B2) eye drops to trigger a reaction that changes the cross-links between and within collagen fibers in the cornea. The stiffening of the corneal tissue is hypothesized to strengthen and stabilize the cornea, thereby flattening the cornea into a more normal shape. This may slow or halt progression of keratoconus. This is an outpatient procedure. There are four types of cross-linking; conventional, where the epithelial layer of the cornea is removed; accelerated, which is similar to conventional but the UV exposure time is decreased; transepithelial, where the epithelial layer of the cornea is not removed; and lastly, partial epithelium-removal, where the epithelial layer of the cornea is only partially removed.
Gene expression profiling for detection of heart transplant rejection
Medica has reviewed gene expression profiling (e.g., AlloMap) for the detection of heart transplantation rejection and has made the following determinations.
- Gene expression profiles for the detection of heart transplantation rejection will be covered for monitoring rejection in heart transplant recipients more than six months post-heart transplant.
- Gene expression profiles for detection of heart transplantation for all other indications is investigative and therefore will not be covered.
Endomyocardial biopsy is the current standard for detecting allograft rejection after transplantation, occurring on a regular basis. As endomyocardial biopsy is invasive and have several limitations, alternative noninvasive techniques to detect rejection have been investigated. The AlloMap (CareDx, Brisbane, CA) test is intended for patients a low probability of moderate to severe acute cellular rejection (ACR) at the time of testing. It incorporates gene expression profiles of 11 informative genes and 9 control genes using a laboratory-generated algorithm to determine an AlloMap score to determine rejection risk in heart transplant patients 55 days or more post-transplant.
The complete text of the policies that apply to the determinations above will be available online or on hard copy:
- See Medica’s coverage policies as of May 1, 2017; or
- Call the Medica Provider Literature Request Line for printed copies of documents, toll-free at 1-800-458-5512, option 1, then option 5, ext. 2-2355.
Effective May 1, 2017:
Medical policies and clinical guidelines to be updated
Medica will soon update one or more utilization management (UM) policies, coverage policies, Institute for Clinical Systems Improvement (ICSI) guidelines, and Medica clinical guidelines, as indicated below. These policies will be effective May 1, 2017, unless otherwise noted.
Coverage policies — New
| Name |
| Corneal Cross-Linking |
| Gene Expression Profiling for Detection of Heart Transplantation Rejection |
Coverage policies — Revised
These versions will replace all previous versions.
| Name |
| Electrical or Electromagnetic Stimulation for Healing of Chronic Wounds |
| Fecal Calprotectin Testing |
| Photodynamic Therapy with Visudyne® (verteporfin) for Ocular Indications |
These documents will be available online or on hard copy:
The importance of screening to prevent colorectal cancer
Colorectal cancer is the second-leading cause of cancer deaths in the United States. It is estimated that about 134,000 people will be diagnosed with colorectal cancer this year and about 49,000 will die from this disease.
But, there’s good news: Screening for colorectal cancer has been made easier. The US Preventive Services Task Force (USPSTF) and the American Cancer Society (ACS) have approved additional testing methods for colorectal cancer. The hope is that these additional screening methods make it easier for providers to encourage patients to be tested.
Screening guidelines
Routine testing should start at the age of 50 and continue to age 75. From 76 to 85 years of age, decisions about screening should be made on an individual basis that takes into account the patient’s overall health and prior screening history.
The following types of screening are available.
| Screening method |
Frequency |
Considerations |
| Fecal immunochemical test (FIT) |
Every year |
Does not require bowel preparation, anesthesia or transportation arrangements to and from the testing. Patients can do the screening sample in the privacy of their own homes. Need one specimen. Do not take specimen from a digital sample. Positive test should be followed up by a colonoscopy.
|
| FIT-DNA |
Every 1 to 3 years |
Does not require bowel preparation, anesthesia or transportation arrangements to and from the testing. Patients can do the screening sample in the privacy of their own homes. Need one specimen. Do not take specimen from a digital sample. Positive test should be followed up by a colonoscopy. |
| Computerized tomography (CT) colonography |
Every 5 years |
Non-invasive. No sedation needed. Requires bowel prep and fasting. Positive test should be followed up by a colonoscopy. |
| Colonoscopy |
Every 10 years |
Requires special prep, including dietary restrictions and fasting. Need sedation and/or anesthesia. Patient must have transportation arranged. Screening and diagnostic follow-up of positive findings can be performed during the same examination. |
| Flexible sigmoidoscopy |
Every 10 years |
Bowel prep needed. Some sedation may be needed. Can be done in the provider’s office with a sigmoidoscopy. If positive findings, the polyps can be removed and biopsied. May also require a colonoscopy if there are positive findings. |
Medica has signed a pledge to have 80 percent of its members screened for colorectal cancer by 2018. In the state of Minnesota, approximately 71 percent of Minnesotans over the age of 50 receive regular colorectal cancer screenings. Medica’s colorectal screening rate measured in 2015 was 52 percent. Providers and plans together should now make every effort to achieve 80 percent by 2018!
Further reference
For more information, refer to the Minnesota Department of Health, USPSTF, ACS or Journal of the American Medical Association (JAMA).
[Return to top]
Pharmacy News
Corrections:
Drug list changes to be eff. April 1 for new prescriptions
Only 2 drug lists will be updated
As a correction to what was published last month, the changes to Medica drug lists that were announced for May 1, 2017, will actually apply beginning April 1, 2017, for new prescriptions. Existing patient prescriptions will not be affected until May 1, 2017, so in essence, these patients are grandfathered 30 days beyond the update's effective date.
In addition, Medica will be making changes in coverage status only to the following drug formularies (drug lists), which again will be effective April 1, 2017, for new prescriptions:
- the 2017 Medica Commercial Large Group Drug List
- the 2017 Medica List of Covered Drugs for Minnesota Health Care Programs (MHCP)
Medica will not make changes effective on either April 1 or May 1 to the Preferred Drug List for individual and family business (IFB) members (“2017 Individual and Family Drug List”) or small group plan members (“2017 Commercial Small Group Drug List”). Also as an update, more about upcoming changes that will apply to Medica Medicare Part D formularies is included down below.
Medica will post changes to its drug formularies on medica.com prior to their effective date. To see the latest Medica drug list changes as well as full drug formularies for each member type, refer to medica.com.
Effective May 1, 2017:
Medica to add new UM policies for medical pharmacy drugs
Medica will soon implement the following new medical pharmacy drug utilization management (UM) policies, effective with May 1, 2017, dates of service. Prior authorization will be required for the corresponding medical pharmacy drugs. These UM changes will apply to relevant prior authorization and pre-payment claims edit policies.
Medical pharmacy drug UM policies – New
Prior authorization will be required.
| Drug code |
Drug brand name |
Drug generic name |
| J9034 |
Benedeka |
bendamustine |
| J2786 |
Cinqair |
reslizumab |
| J9145 |
Darzalex |
daratumumab |
| J9176 |
Empliciti |
elotuzumab |
| J9325 |
Imlygic |
talimogene laherparepvec |
| J2840 |
Kanuma |
sebelipase alpha |
| J2182 |
Nucala |
mepolizumab |
| J9205 |
Onivyde |
irinotecan liposome |
| J9295 |
Portrazza |
necitumumab |
| J9352 |
Yondelis |
trabectedin |
These policies will apply to Medica commercial, Minnesota Health Care Programs (MHCP) and individual and family business (IFB) members, but not to Medica Medicare members. All of these policies will be subject to pre-payment claims edits as well.
The new medical pharmacy drug UM policies above will be available online or on hard copy:
Effective May 1, 2017:
Medica to revise UM policies for medical pharmacy drugs
Medica will soon revise the following medical pharmacy drug utilization management (UM) policies, effective with May 1, 2017, dates of service. The following medications previously assigned a code are being updated to reflect a new code. These UM changes will apply to relevant prior authorization and pre-payment claims edit policies.
Medical pharmacy drug UM policies – Revised
| Drug code |
Drug brand name |
Drug generic name |
Change |
| J7320 |
GenVisc850 |
hyaluronic acid |
Update code from Q9980 to J7320 |
| J7322 |
Hymovis |
hyaluronic acid |
Update code from C9471 to J7322 |
These policies will apply to Medica commercial, Minnesota Health Care Programs (MHCP) and individual and family business (IFB) members, but not to Medica Medicare members. All of these policies will be subject to pre-payment claims edits as well.
The updated medical pharmacy drug UM policies above will be available online or on hard copy:
Effective May 1, 2017:
Upcoming changes to Medica Part D drug formularies
Medica posts changes to its Part D drug formularies on medica.com 60 days prior to the effective date of change. The latest lists will notify Medicare enrollees of drugs that will either be removed from the Medica Part D formulary or be subject to a change in preferred or tiered cost-sharing status effective May 1, 2017. Medica also notifies affected Medica members in their Medicare Pard D Explanation of Benefits (EOB) statements mailed out monthly.
As of March 1, 2017, view the latest Medicare Part D drug formulary changes.
Medica periodically makes changes to its Medicare Part D formularies: the Medica Prime Solution® Part D closed formulary (4-tier + specialty tier) and the Medica DUAL Solution® Part D closed formulary. The Medica Medicare Part D drug formularies are available online or on paper:
Medication request forms
A medication request form should be used when requesting a formulary exception. It is important to fill out the form as completely as possible and to cite which medications have been tried and failed. This includes the dosages used and the identified reason for failure (e.g., side effects or lack of efficacy). The more complete the information provided, the quicker the review, with less likelihood of Medica needing to request more information. To request formulary exceptions, providers can submit an exception form or call CVS Caremark.
[Return to top]
Administrative News
Provider College administrative training topic for March

The Medica Provider College offers educational sessions on various administrative topics. The following class is available by webinar for all Medica network providers, at no charge.
Training class topic
"Resources for Helping Yourself" (class code: RH)
Medica is continually updating services and resources available to network providers. This webinar will walk through self-service options available to providers, including resources on medica.com. These services and resources assist providers in running their offices more efficiently.
Class schedule
| Class code |
Topic |
Date |
Time
|
Notes |
| RH-WM |
Resources for Helping Yourself |
March 27 |
10-11 am |
Class code with "WM" means offered via webinar in March |
For webinar trainings, login information and class materials are e-mailed close to the class date. To ensure that training materials are received prior to a class, providers should sign up as soon as possible.
The time reflected above allows for questions and group discussion. Session times may vary based on the number of participants and depth of group involvement.
Registration
The registration deadline is one week prior to the class date. Register online for the session above.
Reminder on billing for dually eligible patients
As a reminder, the Centers for Medicare and Medicaid Services (CMS) does not allow providers to hold members eligible for both Medicare and Medicaid financially responsible for Medicare Part A and Part B copayments, coinsurance, or deductibles when Medicaid is responsible for payment of such amounts. Also, Medica will not impose cost-sharing in excess of the cost-sharing permitted under Title XIX of the Social Security Act. Providers need to accept Medica’s payment for health services as payment in full, or bill the appropriate state source. The prohibition for collecting Medicare cost-sharing is limited to services covered under Medicare Parts A and B.
Helpful tip on gender-based claim edits for IFB members
Providers can help prevent denials for claims related to services that have been provided to transgender patients, specifically those who are Individual and Family Business (IFB) members. In an effort to reduce the processing of incorrectly coded claims, Medica may deny IFB member claims when there is a gender mismatch between the gender of the individual receiving the treatment or service and the billing code associated with the biological sex that typically receives the service. However, providers can alert Medica to ignore an apparent gender mismatch for a transgender patient by submitting claims with modifier KX (“Requirements specified in the medical policy have been met”) or condition code 45 (“Ambiguous gender category”). Coding with this level of specificity should help avoid delays and claim re-work, and allow for faster claim payment.
Updates to Medica Provider Administrative Manual
To ensure that providers receive information in a timely manner, changes are often announced in Medica Connections that are not yet reflected in the Medica Provider Administrative Manual. Every effort is made to keep the manual as current as possible. The table below highlights updated information and when the updates were (or will be) posted online in the Medica Provider Administrative Manual.
| Information updated |
Location in manual |
When posted |
| In accordance with NOTICE Act, added “Medicare Outpatient Observation Notice” provision requiring hospitals to provide specified notice to members receiving observation services as outpatients |
“Special Contracting Requirements” section, in “Government Program Requirements” subsection, under “Provider Requirements for Medicare, Medicaid and Government Programs” |
January 2017 (effective 3/1/17)
|
For the current version, providers may view the Medica Provider Administrative Manual online.
[Return to top]
SelectCare/LaborCare News
Latest UHC provider bulletin available online
UnitedHealthcare (UHC) has published the latest edition of its Network Bulletin (February 2017). Highlights that may be of interest to LaborCare® network providers include:
- UHC collects HEDIS medical records every year to meet CMS requirements
- Quest Diagnostics runs UHC Worksite Wellness biometrics program – effective as of January 2017
- Revision to immune globulin (IVIG and SCIG) drug policy – effective as of February 2017
- Revision to bariatric surgery medical policy – scheduled for March 2017
View the February 2017 UHC provider bulletin.
[Return to top]